|
As mentioned above, higher flow rates are possible with a standard nasal cannula, but often are not well-tolerated by the patient because of discomfort. Additionally, this system blows cool, dry air that causes nasal mucosal irritation at higher flow rates, which can lead to epistaxis. 1 This is one of the main limitations of low-flow nasal cannula its low-flow state allows for mixing of ambient air with the oxygen source, ultimately resulting in a lower FiO2 delivered to the patient. For example, the FiO2 of a patient receiving 6L via nasal cannula is diluted to approximately FiO2 45%. Although oxygen directly inside the tubing from the wall has a fraction of inspired oxygen (FiO2) of 100%, this mixes with ambient air and dilutes the amount of FiO2 the patient actually receives. A traditional low-flow nasal cannula provides up to 6L/min of flow (though higher rates are possible), which is far from the demand of patients in respiratory distress. When a patient is in respiratory distress, the inspired flow demand can exceed 100L/min. duPont Hospital for Children in Wilmington, Del., and clinical assistant professor of pediatrics at Jefferson Medical College in Philadelphia.Supplemental oxygen is the most common intervention used when managing hypoxic patients and can be easily applied via nasal cannula connected to oxygen from the wall.Īt rest, the inspired flow of a normal respiratory cycle is approximately 30 liters (L) per minute. Stubblefield is a pediatric hospitalist at Nemours/Alfred I. The mechanics of breathing in children with acute severe croup. The Relationship between High Flow Nasal Cannula Flow Rate and Effort of Breathing in Children. The optimal HFNC rate to decrease effort of breathing for children less than 3 years old is between 1.5 and 2 L/kg/min with the greatest improvement expected in children under 5 kg. The authors did not report the fraction of inspired oxygen settings used, the size of HFNC cannulas, or how PRP changed over several days as HFNC was weaned. There was no difference seen between the two HFNC systems in the study. A rate of 2 L/kg per minute was chosen as a maximum a priori as it was judged the highest level of HFNC patients could tolerate without worsening agitation or air leak. Given the similarity in drop in PRP at 1.5 L/kg per minute and 2 L/kg per minute, the authors suggest this flow rate yields a plateau effect and minimal further improvement would be seen with increasing flow rates. Further examining these younger and lighter patients, the greatest reduction in PRP was in the lightest patients (less than 5 kg). 38), with all significant changes being in patients less than 8 kg ( P less than. 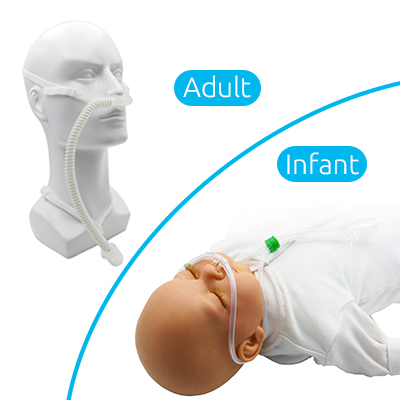
When stratifying the subjects by weight, this effect was not statistically significant for patients heavier than 8 kg ( P =. 001) and a slightly smaller but similar reduction in PRP at 1.5 L/kg per minute. Following the trials, patients remained on HFNC as per usual care with twice-daily PRP measurements until weaned off HFNC.Ī dose-dependent relationship existed between flow and change in PRP, with the greatest reduction in PRP at 2 L/kg per minute flow ( P less than. Each patient received HFNC delivered by both systems in sequence with flow rates of 0.5, 1, 1.5, and 2 L/kg per minute to a maximum of 30 L/min. Thirteen patients had bronchiolitis, three had pneumonia, and five had other respiratory illnesses. Prior data suggested a sample size of 20 would be sufficient to identify a clinically significant effect size. Fifty-four patients met inclusion criteria and 21 were enrolled and completed the study. SynopsisĪ single center recruited patients aged 37 weeks corrected gestational age to 3 years who were admitted to the ICU with respiratory distress. SettingĢ4-bed pediatric intensive care unit in a 347-bed urban free-standing children’s hospital. Single-center prospective observational trial. The authors chose systems from Fisher & Paykel and Vapotherm for their testing. 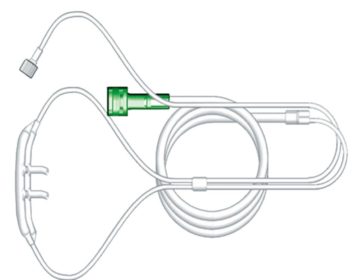
1 An increasing PRP indicates increasing effort of breathing. Placing a manometer in the esophagus allows measurement of the pressure-rate product (PRP), a previously validated measure of effort of breathing computed by multiplying the difference between maximum and minimum esophageal pressures by the respiratory rate. Reliably measuring effort of breathing has proved challenging.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
